More than head support: general interventions to optimize head position
Michelle L. Lange, OTR/L, ABDA, ATP/SMS
Our last Blog addressed some of the causes of poor head position. In this Blog, we will explore general intervention strategies – things to try long before grabbing a specific head support. It is so tempting when we see a client with a sub-optimal head position to immediately try a different head support. However, our solution will be dictated by specific causes. And many of our solutions involve overall client position, not just a head support.
General Interventions include:
- Ensuring the pelvis is in a neutral rotation
- Increase trunk extension and scapular retraction
- Change the impact of gravity on head position
- Refer to neuro-optometrist, as appropriate
Head position is quite dependent upon the position of the trunk and pelvis. If the pelvis is in a posterior tilt, the trunk will be flexed or kyphotic. Due to the flexion of the trunk, the neck will also be flexed and any attempt to right the head will result in neck hyperextension (see figures below). If the pelvis is in an anterior tilt, the trunk will be extended or lordotic. This may lead to hyperextension of the neck as the client attempts to keep the trunk upright and the head balanced. In general, the pelvis should be placed in a neutral alignment, if possible, and the trunk supported in an upright posture. If the shoulders remain protracted or rounded, seating interventions to promote scapular retraction can help the client maintain a more upright head position.

Trunk Flexion is leading to neck hyperextension 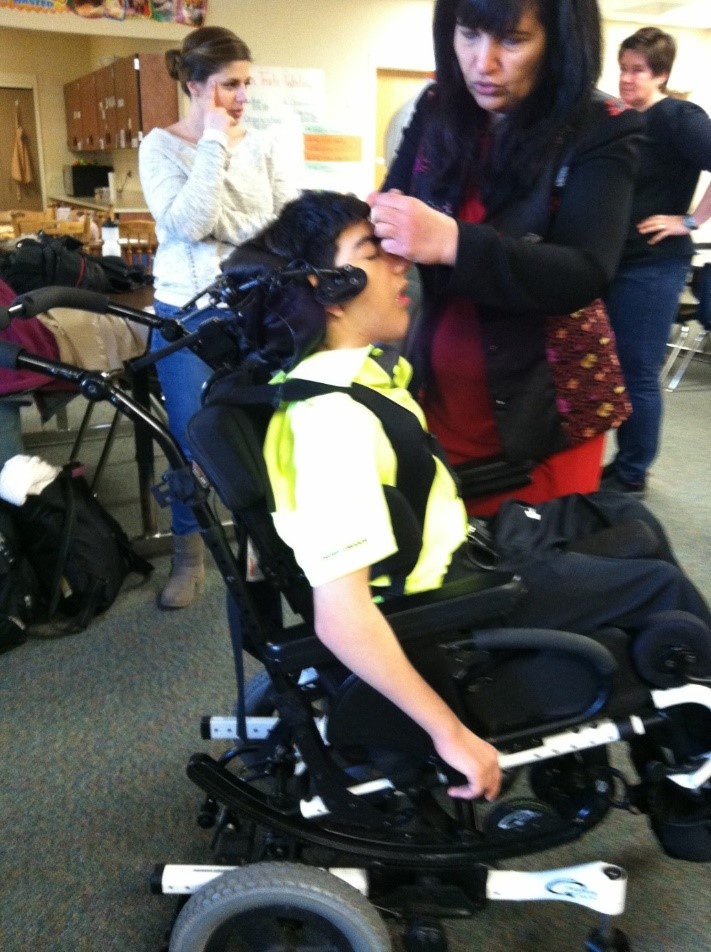
Tightening the shoulder straps extended the trunk and retracted the scapulae, resulting in an aligned neck
For people with decreased head control, gravity can pull the head forward. Opening the seat to back angle or providing some posterior tilt in space can reduce the influence of gravity on head position and facilitate head control. For clients with a non-reducible kyphosis, the seat to back angle can be increased and/or tilt used until the head is over or just behind the pelvis (see figures below). This will allow the client to balance their head over the kyphosis without neck hyperextension. In clients without kyphosis, a significant amount of recline or tilt will often maintain the head in contact with a head support but is not a functional position and may even result in further loss of head control.

Without tilt, this gentleman is looking at his lap due to fixed kyphosis 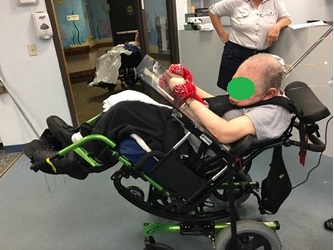
Posterior tilt to allow him to look forward
If the evaluation team suspects that vision is impacting head position, a referral can be made to a Neuro-Optometrist for evaluation and recommendations. Some interventions may improve head alignment, particularly in the case of midline shifts. For clients with Cortical Visual Impairment (CVI), atypical head positions are to be expected, as well as allowed. The client may need to assume a specific position to optimize vision – often with the head slightly forward and/or tilted.
Once head position has been optimized through these strategies, the evaluation team can determine the most appropriate head support. Keep an eye out for our next Blog which will address just that!